Page 41 - DP.qxd
P. 41
In this article’s authors’ dental practice, a 10-year implant
guarantee is offered, linked to a hygiene maintenance
programme. This programme is risk dependent, and patients
are seen between one and four times a year, accordingly. This
programme is complemented with a pre-treatment phase
with the hygiene team. This includes not only mechanical
cleaning and disease control, but also a risk assessment
(plaque control, medical conditions, smoking habit), and
grading of the complexity of implant treatment. Thorough
oral hygiene instruction is given, and the maintenance
programme explained.
After an implant restoration is fitted, the patient has an
appointment with the hygiene team to take baseline probing
measurements, and to demonstrate how best to clean their
new restoration. Any maintenance programme such as this
will reduce the possibility of late complications, by reducing
risk factors but also identifying problems at an early stage.
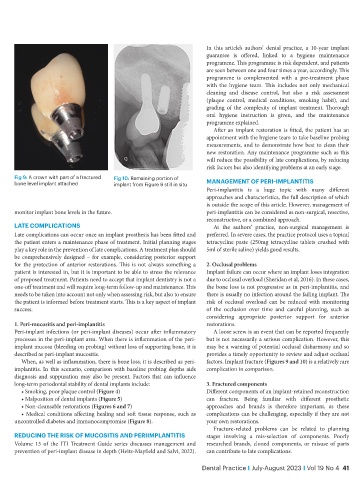
Fig 9: A crown with part of a fractured Fig 10: Remaining portion of
bone level implant attached implant from Figure 9 still in situ management of peRi-impLantitis
Peri-implantitis is a huge topic with many different
approaches and characteristics, the full description of which
is outside the scope of this article. However, management of
monitor implant bone levels in the future. peri-implantitis can be considered as non-surgical, resective,
reconstructive, or a combined approach.
Late compLications At the authors’ practice, non-surgical management is
Late complications can occur once an implant prosthesis has been fitted and preferred. In severe cases, the practice protocol uses a topical
the patient enters a maintenance phase of treatment. Initial planning stages tetracycline paste (250mg tetracycline tablets crushed with
play a key role in the prevention of late complications. A treatment plan should 5ml of sterile saline) yields good results.
be comprehensively designed – for example, considering posterior support
for the protection of anterior restorations. This is not always something a 2. Occlusal problems
patient is interested in, but it is important to be able to stress the relevance Implant failure can occur where an implant loses integration
of proposed treatment. Patients need to accept that implant dentistry is not a due to occlusal overload (Sheridan et al, 2016). In these cases,
one-off treatment and will require long-term follow-up and maintenance. This the bone loss is not progressive as in peri-implantitis, and
needs to be taken into account not only when assessing risk, but also to ensure there is usually no infection around the failing implant. The
the patient is informed before treatment starts. This is a key aspect of implant risk of occlusal overload can be reduced with monitoring
success. of the occlusion over time and careful planning, such as
considering appropriate posterior support for anterior
1. Peri-mucositis and peri-implantitis restorations.
Peri-implant infections (or peri-implant diseases) occur after inflammatory A loose screw is an event that can be reported frequently
processes in the peri-implant area. When there is inflammation of the peri- but is not necessarily a serious complication. However, this
implant mucosa (bleeding on probing) without loss of supporting bone, it is may be a warning of potential occlusal disharmony and so
described as peri-implant mucositis. provides a timely opportunity to review and adjust occlusal
When, as well as inflammation, there is bone loss, it is described as peri- factors. Implant fracture (Figures 9 and 10) is a relatively rare
implantitis. In this scenario, comparison with baseline probing depths aids complication in comparison.
diagnosis and suppuration may also be present. Factors that can influence
long-term periodontal stability of dental implants include: 3. Fractured components
• Smoking, poor plaque control (Figure 4) Different components of an implant-retained reconstruction
• Malposition of dental implants (Figure 5) can fracture. Being familiar with different prosthetic
• Non-cleansable restorations (Figures 6 and 7) approaches and brands is therefore important, as these
• Medical conditions affecting healing and soft tissue response, such as complications can be challenging, especially if they are not
uncontrolled diabetes and immunocompromise (Figure 8). your own restorations.
Fracture-related problems can be related to planning
Reducing the Risk of mucositis and peRiimpLantitis stages involving a mis-selection of components. Poorly
Volume 13 of the ITI Treatment Guide series discusses management and researched brands, cloned components, or misuse of parts
prevention of peri-implant disease in depth (Heitz-Mayfield and Salvi, 2022). can contribute to late complications.
Dental Practice i July-August 2023 i Vol 19 No 4 41